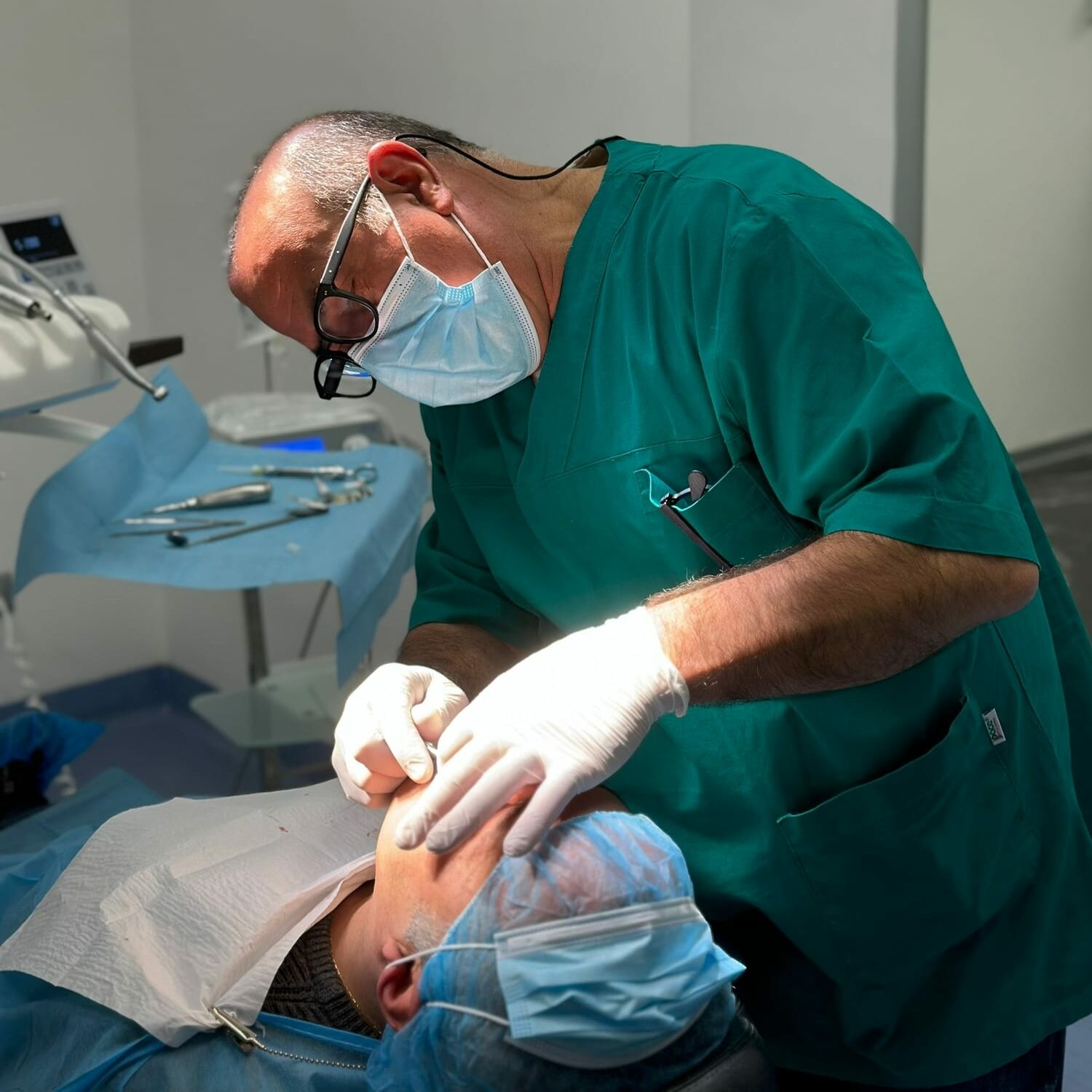
We have listed peri-implantitis as the cause of the loss of a dental implant. Let’s try to understand specifically what this particular pathology is so insidious for patients who have undergone an implantology intervention.
What is peri-implantitis?
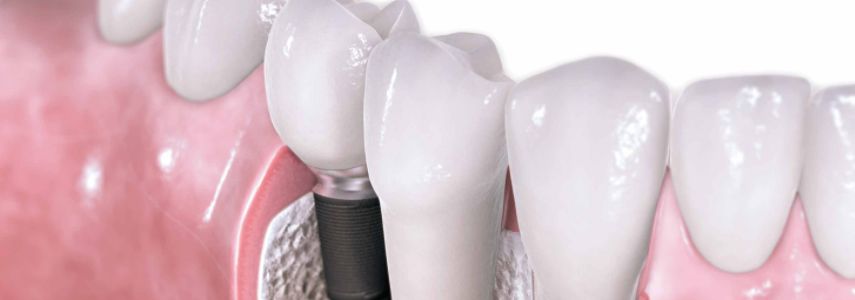
Periimplantitis is nothing more than an infection of bacterial origin, what distinguishes it from the rest of the other infections is that it has the peculiarity of developing around the dental implant. The infection actually undermines the maxillary bone in which the implant is inserted, jeopardizing the stability of the prosthesis itself.
Periimplantitis is analogous to periodontitis and has the same consequences. This type of pathology is the consequence of the proliferation, in the area adjacent to the implant, of Gram negative anaerobic bacteria, the same type of bacteria responsible for periodontitis. For this reason, one of the main contraindications for those who decide to undergo an implantology intervention is the presence of ongoing infections, because the bacteria could easily colonize even the part adjacent to the implant.
How to recognize the symptoms of peri-implantitis?
The correct course following an implantology operation does not foresee any contraindications, so if everything is proceeding for the best, the patient has no pain and no discomfort. The alarm bells are therefore quite evident and it is important not to underestimate them.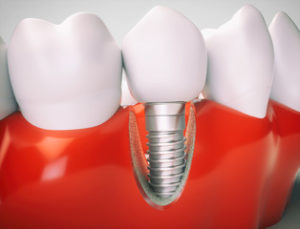
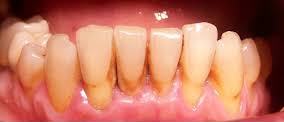
Redness of the gums near the implant
The redness and swelling of the gums is the first symptom of an ongoing infection, the gingival tissue around the implant becomes more sensitive and is also often subject to bleeding.
Presence of pus close to the implant
If the infection is already at an advanced stage, a leak of pus is likely to form in the affected area.
Pain or discomfort
A dental implant, as we have already said, should not bother you. So the presence of pain during chewing or touch is a clear symptom of an abnormal condition.
Plant mobility
In this case it may be already too late, if the implant is no longer stable it is likely that the maxillary bone is already seriously compromised.
None of these conditions should be neglected in the least, it is important to contact your dentist immediately for an accurate diagnosis and an adequate treatment plan.
Peri-implantitis can also occur years after the insertion of the implants and very often it is the direct consequence of poor oral hygiene and lack of care of the implants.
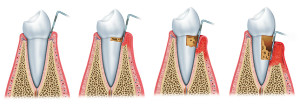
We can therefore distinguish an early peri-implantitis from a late one: in the first case the infection attacks the implant before the osseointegration phase, in the second case the peri-implantitis arises after already osseointegration.
Is there a cure for peri-implantitis?
 In general, if peri-implantitis is not in an advanced stage, it can be cured by eliminating bacteria and treating the infection. In severe cases, infection removal therapy may involve minor surgery.
In general, if peri-implantitis is not in an advanced stage, it can be cured by eliminating bacteria and treating the infection. In severe cases, infection removal therapy may involve minor surgery.
The best cure for fighting peri-implantitis remains prevention. Taking care of the dental implants, not neglecting oral hygiene, following the advice that the dentist provides in the post-surgery procedure, the best solutions remain to avoid post-surgery complications.